If you are reading this, you have likely just been told that your pregnancy is affected by Spina Bifida (SB). Like most women receiving this unexpected diagnosis, you want to know what it is, and what to expect.

What is Spina Bifida?
Spina Bifida describes a group of neural tube defects (NTD’s) that occur when the baby’s developing spine (neural tube) fails to close properly. When most people speak of SB, they are referring to the most common and also most severe form, called myelomeningocele, which causes the spinal nerves to bulge through an opening in the back. Myelomeningocele usually occurs in the lowest part of the spine but can occur at any level. Spina Bifida is the most common permanently disabling birth defect that is compatible with living into adulthood.

What causes SB?
There is no single known cause for SB. It is due to a complex interaction of both genetic and environmental factors occurring very early in the pregnancy (by the 4th week). The genetic factors that can cause SB are not well known. Research has shown that supplementation of folic acid ( a “B” vitamin) reduces the risk of having a pregnancy affected by SB. However, many people who take folic acid still have babies with SB, and women who did not take folic acid still have healthy babies. No one knows why. It just happens. This means that there is still much to learn about the causes of SB, and it is nobody’s fault.
How is SB diagnosed during pregnancy?
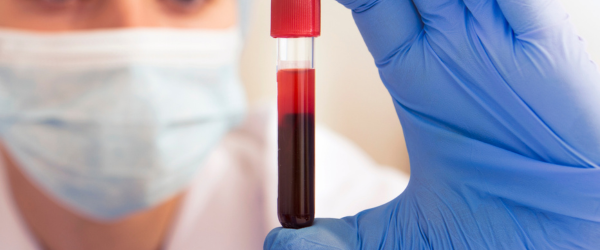
Maternal Serum Alpha – Fetoprotein (MSAFP)
Maternal Serum Alpha – Fetoprotein (MSAFP) also known as triple test or quad test, is a blood test performed between the 15th and 20th weeks of pregnancy to determine if there is a higher risk for NTD. MSAFP testing measures the level of a protein (AFP) made by the fetus and placenta. Small amounts of this protein normally cross the placenta into the maternal bloodstream, but when very high levels cross, it could be that the fetus has an NTD. However, MSAFP testing is not used as a diagnostic tool but rather as an indicator that further testing is needed, because the test is not specific for SB, and because high MSAFP may be present for a number of other reasons.

Ultrasound
Ultrasound is the primary diagnostic tool for prenatal diagnosis of SB and other NTD’s. It is a non-invasive technique that produces an image of the fetus. It can be used to identify many different problems in fetuses, but can also be used to identify important characteristic signs of SB in both the brain and spine. Cranial markers include the lemon sign (abnormal shape of fetal skull), the banana sign (crowding of the cerebellum in the back part of the head), and hydrocephalus (abnormally large ventricles or fluid spaces in the brain). The normal fetal spine resembles a string of pearls. An SB spine will appear as a string of pearls with some broken or missing pieces.
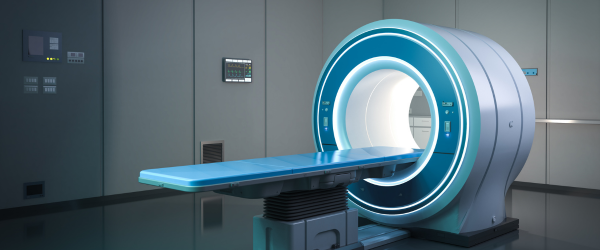
Fetal MRI
Fetal MRI may be recommended after the diagnosis is made through ultrasound to determine severity of SB. MRI is a powerful technology that uses magnetic imaging (not radiation) to give better pictures of the fetal spinal cord and spinal nerves. Through MRI, the doctors can see the size and extent of the SB. This information helps them explain the diagnosis and prognosis (expected long term condition) in greater detail. Fetal MRI is not necessary for all pregnancies affected by SB though, particularly when the ultrasound images are good
What medical issues do people with SB encounter?
People with SB have a number of medical issues to deal with throughout their lives.
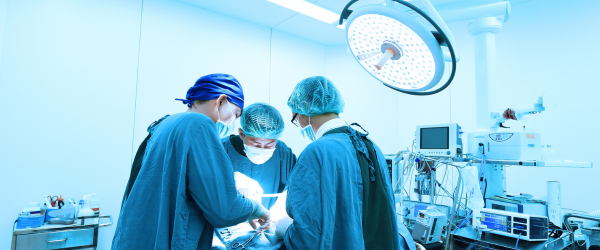
Surgical
Open SB lesions need to be surgically closed (usually within 72 hours after birth) to prevent infection and further damage to the spinal cord.

Learning Difficulties
Although most individuals with SB have normal IQ scores, they may have learning difficulties; but these can often be addressed when parents and teachers understand the issues and work together.

Hydrocephalus
Hydrocephalus is an excessive amount of cerebral spinal fluid (CSF) collecting in the ventricles of the brain. It occurs in approximately 80% of patients with SB. Sometimes it occurs before birth, but most often it occurs after the back has been closed. Hydrocephalus is usually treated by surgery to place a hollow tube called a ventriculoperitoneal (VP) shunt that transfers the fluid from the head to an empty space in the abdomen in order to prevent brain damage. (Please see the SBA’s info sheet on hydrocephalus and shunts for more information).

Bowel and Bladder Disorders
Neurogenic (dysfunctional) bowel and bladder is caused by damage to the nerves that control the function of the bladder and the bottom section of bowel and anus. In recent years, a number of treatments have been developed which allow individuals to achieve varying levels of functional continence. (Please see the SBA’s information sheet on urologic care and management for more information).

Mobility Issues
Many people with SB face mobility issues, which are dependent on the spinal level of the SB lesion. Most children are able to walk (though usually with the aid of orthopedic bracing and often with assistive devices such as crutches). Some are full-time walkers, but many walk short distances and choose a wheelchair for long distances. It is generally only those with thoracic or high lumbar spinal lesions who end up using the wheelchair as their only method of mobility.
Every individual with SB is affected differently, and it is impossible to fully predict a child’s outcome before or at birth. Outcomes have improved over the past 50 years due to medical advancements. In addition, cultural attitudes toward individuals with disabilities have also changed, resulting in improved services.
While some individuals with SB have significant disabilities, others are less severely affected. Many attain advanced education, and have careers and families of their own. They become doctors, teachers, artists, athletes, and parents. Spina Bifida is only one part of their lives; it does not define them.
What are the choices for women carrying fetuses with SB?
To learn the most about the prognosis for YOUR pregnancy, it is recommended that you meet with a pediatric neurosurgeon and/or SB clinic as soon as possible. You will also need to meet with a maternalfetal specialist or perinatologist to closely follow your pregnancy. You may also meet other specialists who care for people with SB. Use these appointments to learn as much as you can. After you have gathered enough information to understand the immediate and long term implications of SB, consider the choices available to you—terminating the pregnancy, prenatal or postnatal surgery, or adoption—what matters is that you make an informed choice about what works best for you and your family.
Prenatal or Postnatal Surgery
For pregnancies diagnosed earlier than 25 weeks gestation, in-utero fetal surgery may be an option to close the baby’s back before birth. There are potential risks and benefits of fetal surgery, and it is not appropriate for all women.
For those who choose and qualify, an immediate referral must be made to a medical center where the operation is performed. Because fetal surgery is not standard practice at this time, most newborns with SB require surgery shortly after birth to prevent infection and further spinal cord damage.